Delayed Diagnosis of Pulmonary Histoplasmosis in an Immunocompetent Young Asthmatic Female from Florida, a Non-Endemic Area for Histoplasma Capsulatum
Meghana Gudala and Satyanarayan Hegde
DOI10.21767/2471-8521.100001
Meghana Gudala1* and Satyanarayan Hegde2,3
1Osmania Medical College, India
2Pediatric Pulmonary Medicine, University of Chicago & Comer Children’s Hospital, 5841, S. Maryland Ave, MC 4064, Room WP-C-150A, Chicago, IL 60637, USA
3University of Florida, Gainesville, USA
- *Corresponding Author:
- Satyanarayan Hegde
Pediatric Pulmonary Medicine
University of Chicago & Comer Children’s Hospital
5841, S. Maryland Ave, MC 4064, Room WP-C-150A
Chicago, IL 60637, USA
E-mail: shegde@bsd.uchicago.edu
Tel: 773-702-6178
Received date: September 01, 2015; Accepted date: September 27, 2015; Published date: October 01, 2015
Citation: Gudala M, Hegde S. Delayed Diagnosis of Pulmonary Histoplasmosis in an Immunocompetent Young Asthmatic Female from Florida, a Non-Endemic Area for Histoplasma capsulatum. Med Mycol Open Access. 2015, 1:1. doi: 10.21767/2471-8521.100001
Copyright: © 2015 Gudala M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Pulmonary histoplasmosis is caused by Histoplasma capsulatum, a dimorphic fungus. We report an unusual case of pulmonary histoplasmosis in an immunocompetent 16 year old African American female from Florida. She had history of asthma and presented with recurrent episodes of difficulty breathing and chest tightness however with no wheezing. Multiple medications including systemic steroids and hospitalizations which focused on her asthma symptoms could not improve her condition. Her family history was suggestive of sarcoidosis and lymphoma, whereas her travel history revealed trips to caves in Tennessee few years previously. Extensive workup that included chest x
rays, computerized tomography (CT) scans, spirometry, bronchoscopy with broncho alveolar lavage (BAL), lymph node biopsy, wedge biopsy of the lung, serology for histoplasma, Quantiferon gold test for tuberculosis were performed as the patient’s clinical presentation unfolded over 12 months. Additionally there were other complicating psychosocial factors such as obesity and anxiety. The wedge biopsy of the lung established the final diagnosis of pulmonary histoplasmosis. This case underscores the importance of keeping broad differential diagnoses and obtaining careful history in an asthmatic patient.
Introduction
Histoplasma capsulatum is a dimorphic fungus found in the soil in the mycelial form and in the tissues in the yeast form. It produces conidia, which are commonly found in moist, acidic soils contaminated with bird and bat excreta [1,2]. H. capsulatum var capsulatum is the most common variety causing histoplasmosis worldwide including United States [3,4]. A less common variety seen which is mostly endemic in western and central regions of sub-Saharan Africa is Histoplasma capsulatum var duboisii which is less common elsewhere and if present is mostly because it is imported. Ecology and pathogenesis of Histoplasma capsulatum var duboisii is not well known [5].
Histoplasmosis is the most common endemic mycosis in North America affecting up to 95% of inhabitants of certain geographic areas in the Ohio and Mississippi river valleys [6]. Cases may usually be caused by disturbance of soil contaminated with H. capsulatum [7] or by visiting bat caves [8]. Infection occurs by inhalation of the microconidia, which are readily airborne and able to reach small bronchi and alveoli [9]. If they are inhaled, the organism is ingested by tissue macrophages. It might then proliferate within macrophages, spread to regional lymph nodes or disseminate via hematogenous or lymphatic routes until the development of specific cell-mediated immunity [10-12]. If they evade nonspecific lung defenses, localized and patchy bronchopneumonia results [13]. With low inoculum exposure, otherwise healthy persons remain asymptomatic but with large inoculum or impaired immunity, patients can develop a severe and potentially fatal acute diffuse pulmonary disease [14,15].
In endemic areas, the population is infected and probably reinfected multiple times but the vast majority of both primary infections and reinfections are clinically silent [16]. Reactivation of the infection is seen in patients who are immunocompromised and increasingly cases are recognized in patients receiving treatment with tumor necrosis factor inhibitors [17]. Chronic pulmonary histoplasmosis is seen in patients with underlying lung disease and the presentation is similar to tuberculosis. Underlying lung disease includes emphysema, vascular compromise, tissue necrosis and fibrosis. Inflammation is disproportionate to the fungal burden suggesting that hypersensitivity to fungal antigens may play a role in the pathogenesis [18]. Treatment with corticosteroids has been associated with progressive disseminated histoplasmosis [19]. We report a case of pulmonary histoplasmosis in an otherwise immunocompetent young asthmatic female from non-endemic area, who was receiving corticosteroids for symptoms attributed to asthma.
Case Presentation
A 16 year old African American female from Florida was first seen at a tertiary pediatric pulmonary clinic for complaints of difficulty in breathing (DIB) and chest tightness (Table 1). This patient has had multiple emergency department (ED) visits and hospitalizations during the previous year for asthma type symptoms, causing her to miss 25 days of school. She was diagnosed with asthma at age 10 years, and was doing well until age 14. Since then she had multiple episodes of DIB and chest tightness not associated with wheezing. She had been using albuterol 3-4 times/week and was also treated with oral and inhaled steroids, which did not improve her symptoms. She was seen by various specialists, including ear, nose and throat (ENT) specialist and an allergist. Her reported triggers for respiratory symptoms included chemical sprays, smells from cooking and perfumes. She developed hoarseness of voice which kept waxing and waning in severity. Her past medical history included pneumonia and sinusitis, but no history of eczema. Her surgical history included adenotonsillectomy, pressure equalizing (PE) tube insertion and surgery on her knee. Father had history of sarcoidosis and lymphoma.
| Presenting symptoms | Asthma like syndrome |
|---|---|
| Pulmonary | Difficulty in breathing (DIB), chest pain |
| Allergy | Reported allergy to perfumes, cooking smells and chemicals; Sensitized to weeds and House dust mite (HDM) |
| Gastro-intestinal | Dysphagia |
| Neurology | Headache , tingling sensation, involuntary movements |
| Psychiatry | Falling school grades, Depression |
| General | Obesity , Fever |
Table 1: History and symptoms.
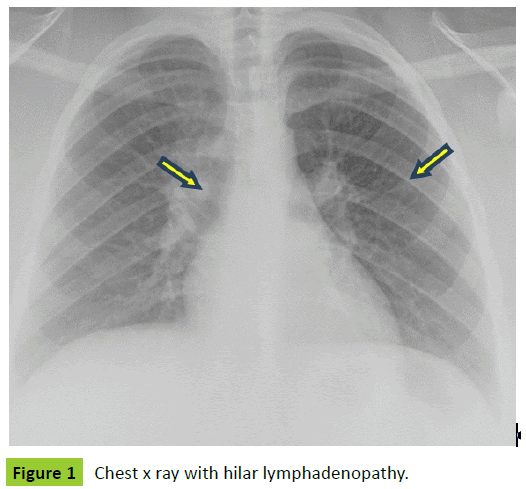
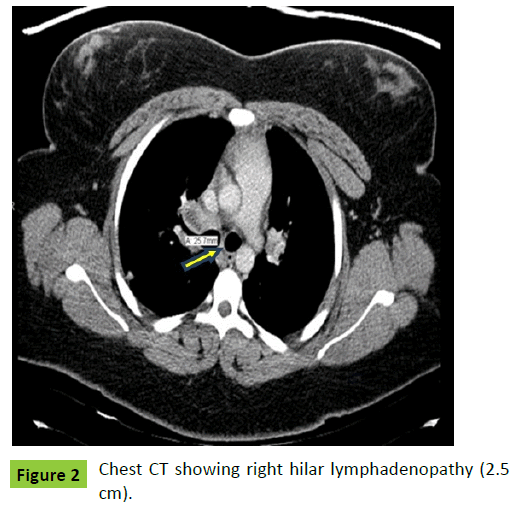
On review of systems, she was negative for wheezing and coughing. On physical examination she was obese with normal bilateral air entry and no adventitious sounds on lung auscultation. Workup included chest radiographs which was suggestive of hilar lymphadenopathy (Figure 1) and spirometry which was normal (Table 2). She was presumptively treated for asthma with Asmanex (Mometasone furoate). Her labs showed normal complete blood count (CBC) and elevated IgE at 540 IU/l. Allergy skin prick test revealed sensitization to house dust mite (HDM), cockroaches and weeds. Radio allegro sorbent test (RAST) showed sensitization to cats, dogs and HDM. Her chest computerized tomography (CT) scan showed right paratracheal and hilar lymphadenopathy with calcifications (Figure 2). A month later, she was hospitalized with difficulty breathing and chest tightness when she also developed fever, sore throat and dysphagia. Work up in the hospital was as follows: Normal bronchoscopy. Broncho-alveolar lavage (BAL) (specific site not given) just showed mild acute and chronic inflammation with 50% lymphocytes and grocott’s methenamine silver (GMS) stain was negative. Polymerase chain reaction (PCR) test was not done on the sample. A fine needle aspiration of either a right hilar or paratracheal lymph node showed just benign mixed lymphoid sampling without granuloma or fibrosis. Cell block was insufficient for further testing and no GMS stain done. A right lower lobe transbronchial biopsy showed mostly bronchial tissue with changes consistent with history of asthma with peribronchial smooth muscle hypertrophy. Again no granulomas or significant inflammation was seen and GMS stain was not done. Esophagoscopy was performed for dysphagia which suggested reflux esophagitis. Her C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) were elevated and Quantiferon gold test for tuberculosis negative. Histoplasma complement fixation test showed results as mycelia<1:8, yeast: 1:32 which is positive for yeast. Histoplasma antigen in urine was negative.
| Serial Spirometry | Normal |
| Exhaled Nitric Oxide | Normal |
| Chest-X-Ray and CT scan | Mediastinal and Hilar Lymphadenopathy; Pulmonary nodules |
| Upper GI endoscopy | Normal |
| Brain MRI | Normal |
| Bronchoscopy | Normal |
| Broncho-alveolar lavage (BAL) | Normal |
| Transbronchial biopsy | Nonspecific inflammation, Peribronchial smooth muscle hypertrophy |
| Thoracoscopic lung biopsy | Granuloma, GMS positive yeast |
| IgE | Elevated |
| Serology | Positive for Histoplasma |
| Urine antigen | Negative for Histoplasma |
Table 2: Investigation findings.
Over next few months, she continued to have recurrent DIB, chest pain and dysphagia. She also developed new symptoms such as jerking involuntary movements in upper limbs, head ache and fatigue. She also reported falling school grades and visual disturbances. Neurology referral was made in view of her new symptoms and magnetic resonance imaging (MRI) scan was normal. She was hospitalized again in three months with DIB along with new onset pleuritic chest pain. Repeat spirometry was normal again and repeats CT scan showed persistent and multiple enlarged mediastinal and hilar lymph nodes some of which had calcifications. There was also a calcified granuloma in the left lung apex and a new right sided sub-pleural nodule with localized air trapping. She was started on proton pump inhibitors (PPI’s) for her dysphagia and chest pain. Patient discontinued PPI’s on her own as there was no therapeutic response. In view of her falling school grades, unexplained multiorgan symptoms and recurrent healthcare utilization, a psychiatry referral was made for suspected anxiety and depression. Pending psychiatry evaluation, a video assisted thoracoscopic (VATS) lung and lymph node biopsy was performed. The thoracoscopic inspection revealed nodular lung on the pleural surface and lung biopsy included right upper lobe wedge excision. This showed noncaseating granuloma (Figure 3) and GMS (Figure 4) and periodic acid schiff (PAS) stains positive yeast establishing the diagnosis of histoplasmosis. Acid fast bacillus (AFB) testing for tuberculosis was negative on the sample. Interestingly the sites of the biopsies done earlier were also sampled at this time (right lower lobe transbronchial biopsy sample) and again were negative for any changes associated with histoplasmosis which included negative GMS and PAS stains. In the meantime patient was also referred to Pediatric Infectious disease department in view of possible histoplasma infection. Further history at this stage, revealed multiple trips to caves in Tennessee and exposure to bats in the previous 5 years. Travel history also included visit to Missouri, Mississippi, Washington D.C, and a cousin in a prison. She improved dramatically when appropriate therapy for histoplasmosis was initiated. Her final treatment included Itraconazole for 12 weeks according to Infectious Diseases Society of America (IDSA) guidelines.
Discussion
Histoplasmosis can be classified into a spectrum of clinical diseases which includes acute pulmonary infiltration with or without lymph nodes enlargement, chronic cavitary lung disease, arthralgia, arthritis, pericarditis, fibrosing mediastinitis, granulomatous mediastinitis and widespread disseminated infection involving skin, liver, spleen, adrenal and central nervous system [20]. Both Chronic pulmonary and disseminated histoplasmosis are more usually reported in immunosuppressed and are major opportunistic infections in HIV/AIDS [18,21], organ transplant recipients [22] and patients on immunosuppressive therapy such as tumor necrosis factor inhibitors [23-25]. However there has been a case of acute disseminated histoplasmosis reported in a 13 year old immunocompetent subject [26]. In immunocompetent subjects, disease is usually self-limited or subclinical. But in some cases, depending on the duration of exposure, delay in diagnosis, and host response, the evolution may be unfavorable [27]. There has also been a case of severe pulmonary histoplasmosis reported in a 15 year old immunocompetent patient [28]. Therefore it is very important to rule out histoplasmosis even in immunocompetent patients.
A closer look at the previously reported cases with similar presentation gives us a great insight. We refer to a 14 year old white male from histoplasma endemic area of Missouri, who had underlying asthma and presented with history of cough initially that was presumptively treated with steroids and albuterol for his asthma [29]. He later complained of worsening cough, pleuritic chest pain and dysphagia, presentation very similar to our case. Since he was from endemic area, histoplasmosis was high on differential and treatment was initiated despite negative histoplasma antibody testing and the patient improved. Another reported case of pulmonary histoplasmosis involves a 15 year old male patient with pulmonary tuberculosis who presented with chronic productive cough [28]. Unfortunately his histoplasmosis was not diagnosed and he died within seven days of inpatient admission and diagnosis was made on autopsy. The third case of acute disseminated histoplasmosis was in a 13 year old immunocompetent boy who presented with dry cough and dyspnea for one month [26]. Extensive work up established the diagnosis and he made complete recovery with treatment.
Our case was complicated by asthma-like symptoms without wheezing. Histoplasmosis is not a reportable condition in Florida, and is often overlooked in the workup of pulmonary or infectious diseases. Skin test reactivity is average only 4.7% in navy recruits from Florida6. Overlooked is that H. capsulatum can be found in caves in Florida [30], providing opportunity for exposure. Our patient reported visiting caves in Tennessee: an endemic area, which would be a likely source for her exposure. This case illustrates the importance of a careful travel history when evaluating patients with clinical findings suggestive of histoplasmosis. The presence of calcified mediastinal lymphadenopathy is highly suggestive of histoplasmosis in this case. Failure to consider histoplasmosis in patients from non-endemic areas is a common cause for missing a diagnosis [31], which can result in serious consequences including death [32]. We postulate that repeated exposure to systemic and inhaled corticosteroids may have prevented her from recovering from pulmonary histoplasmosis without therapy.
When histoplasmosis is considered, the diagnosis can be established rapidly in most patients. We suggest that histoplasmosis should be suspected whenever patients present with pneumonia with mediastinal or hilar lymphadenopathy, pulmonary nodules, cavitary lung disease, pericarditis and dysphagia. All these manifestations place pulmonary histoplasmosis in the differential along with tuberculosis, sarcoidosis and malignancy [33]. It is especially important to rule out histoplasmosis in the evaluation of sarcoidosis, as treatment with corticosteroids or other immunosuppressive therapy often leads to progressive dissemination in patients with pulmonary histoplasmosis [34].
This case illustrates the value of serologic tests in the evaluation for pulmonary histoplasmosis. Antigen detection also is invaluable in diagnosis of pulmonary histoplasmosis [35] but was negative in in this patient when tested for urine histoplasma antigen. Recently PCR methods have been in use which not only helps to diagnose histoplasmosis rapidly but also to differentiate from other fungal infections [36]. PCR can be applied to various tissue and fluid specimens with rapid yield of results. They are valuable, as culture methods-the other means for testing are laborious, protracted and carry safety hazard for laboratory personnel. In a recent study a real time PCR assay which was done directly from clinical specimens has showed sensitivity and specificity of 73% and 100% respectively for detecting Histoplasma capsulatum [37]. Earlier consideration of histoplasmosis in the differential diagnosis and serologic and antigen testing and intervention with PCR methods could have shortened the course and reduced cost associated with repeated hospitalizations and diagnostic testing.
Another interesting finding in this patient is the negative result for histoplasma on biopsy earlier followed by positive result later. The initial transbronchial biopsy specimen from right lower lobe was too small to detect histoplasma infection. However, when the wedge biopsy of the same location was done later on during VATS, it was negative as well for histoplasma. This was when histoplasma infection was detected in the right upper lobe. Infection in the lung was perhaps localized to right upper lobe and hence transbronchial biopsy of right lower lobe did not reveal any granuloma. The right lower lobe was targeted initially based on the radiological findings. However the histoplasma antigen test in the urine around the same time was negative ruling out active infection. We therefore postulate some reasons as to why it was negative earlier but became positive later. We suggest this could be reactivation from dormant infection in the lymph nodes following repeated corticosteroid course. This could also be because of recurrent infection. Since the patient was in Florida throughout her course of presentation, there might have been a re-exposure to the fungus from the soils in Florida, even though patient doesn’t provide any history of cave exploration. As suggested above, there have been cases of histoplasma infection after cave exploration in Florida [30].
In conclusion, it is important to consider the diagnosis in patients with compatible illnesses within and outside endemic areas for histoplasmosis. Our case highlights the importance of clinical expertise in complex cases. The complex interplay between patient reported history, radiological and other objective findings may not always follow text book descriptions. In this case, a repeat chest CT scan showed new lung lesions which prompted thoracoscopic lung biopsy that ultimately clinched the diagnosis. Patient’s health insurer initially refused to cover repeat chest CT as there was no “appropriate indication”. The patient’s treating physician had to speak to a peer reviewer authorized by the insurance company to obtain prior authorization for the CT scan. Without the repeat CT scan, patient’s diagnosis would certainly have been missed with potentially disastrous consequences for the patient.
Failure to diagnose histoplasmosis can result in progressive disease in patients with underlying immunodeficiency caused by the treatment with corticosteroids for a suspected inflammatory cause for the lung disease. The workup for suspected histoplasmosis should include test for antibodies and antigens. Examination of tissue by cytopathology, histopathology, and culture should be done in more severe cases and in those with negative results for antigen or antibody in which another cause has not been established.
Acknowledgements
We would like to express our gratitude to Dr. L. Joseph Wheat, (Mira Vista Diagnostics) for his thoughtful reviews of earlier draft of the manuscript and for his valuable suggestions and contributions.
References
- Sorley DL, Levin ML, Warren JW, Flynn JP, Gersenblith (1979) Bat-associated histoplasmosis in Maryland bridge workers. Am J Med 67: 623-626.
- Addington WW (1967) The ecology of histoplasmosis. Am J Med Sci 253: 687-696
- Wheat LJ, Kauff man CA (2003) Histoplasmosis. Infect Dis Clin North Am 17: 1-19.
- Wheat LJ (2006) Histoplasmosis: a review for clinicians from non-endemic areas. Mycoses 49: 274-282.
- Manfredi R, Mazzoni A, Nanetti A, Chiodo F (1994) Histoplasmosiscapsulati and duboisii in Europe: the impact of the HIV pandemic, travel and immigration. Eur J Epidemiol 10: 675-681.
- Edwards LB, Acquaviva FA, Livesay VT, Cross FW, Palmer CE (1969) An atlas of sensitivity to tuberculin, PPD-B, and histoplasmin in the United States. Am Rev Respir Dis 99: 1-132.
- Stobierski MG, Hospedales CJ, Hall WN, Robinson-Dunn B, Hoch D, et.al. (1996) Outbreak of histoplasmosis among employees in a paper factory-Michigan, 1993. J ClinMicrobiol 34: 1220-1223.
- Sacks JJ, Ajello L, Crockett LK (1986) An outbreak and review of cave-associated histoplasmosis. J Med Vet Mycol 24: 313-325.
- Valdez H, Salata RA (1999) Bat-associated histoplasmosis in returning travelers: case presentation and description of a cluster. J Travel Med 6: 258-260.
- Goodwin RA, Des Prez RM (1978) Histoplasmosis. Am Rev Respir Dis 117: 929-956.
- Goodwin RA, Loyd JE, Des Prez RM (1981) Histoplasmosis in normal hosts. Medicine (Baltimore) 60: 231-266.
- Spivak H, Schlasinger MH, Tabanda-Lichauco R, Ferstenberg H (1996) Small bowel obstruction from gastrointestinal histoplasmosis in acquired immune deficiency syndrome. Am Surg 62: 369-372.
- Procknow JJ, Page MI, Loosli CG (1960) Early pathogenesis of experimental histoplasmosis. Arch Pathol 69: 413-426.
- Kataria YP, Campbell PB, Burlingham BT (1981) Acute pulmonary histoplasmosis presenting as adult respiratory distress syndrome: effect of therapy on clinical and laboratory features. South Med J 74: 534-537.
- Wynne JW, Olsen GN (1974) Acutehistoplasmosis presenting as the adult respiratory distress syndrome. Chest 66: 158-161.
- Goodwin RA Jr, Shapiro JL, Thurman GH, Thurman SS, DesPrez RM (1980) Disseminated histoplasmosis: clinical and pathologic correlations. Medicine (Baltimore) 59: 1-33.
- Wallis RS, Broder M, Wong J, Lee A, Hoq L (2005) Reactivation of latent granulomatous infections by infliximab. Clin Infect Dis 41: 194-198.
- Goodwin RA Jr, Owens FT, Snell JD, Hubbard WW, Buchanan RD, et al. (1976) Chronic pulmonary histoplasmosis. Medicine (Baltimore) 55: 413-452.
- Dismukes WE, Royal SA, Tynes BS (1978) Disseminated Histoplasmosis in Corticosteroid-Treated Patients: Report of Five Cases. JAMA 240: 1495-1498.
- Wheat LJ, Wass J, Norton J, Kohler RB, French ML (1984) Cavitaryhistoplasmosis occurring during two large urban outbreaks. Analysis of clinical, epidemiologic, roentgenographic and laboratory features. Medicine (Baltimore) 63: 201-209.
- Goodwin RA Jr, Snell JD Jr (1969) The enlarging histoplasmoma. Concept of a tumor-like phenomenon encompassing the tuberculoma and coccidioidoma. Am Rev Respir Dis 100: 1-12.
- Cuellar-Rodriguez J, Avery RK, Lard M, Budev M, Gordon SM, et al. (2009) Histoplasmosis in solid organ transplant recipients: 10 years of experience at a large transplant center in an endemic area. Clin Infect Dis 49: 710-716.
- Ciulla T, Piper H, Xiao M, Wheat LJ (2001) Presumed ocular histoplasmosis syndrome: update on epidemiology, pathogenesis, and photodynamic, antiangiogenic, and surgical therapies. CurrOpin Ophthalmol.12: 442-449.
- Deepe GS Jr, Bullock WE (1988) Histoplasmosis: A granulomatous inflammatory response. In: Gallin JI, Goldstein IM, Snyderman R (eds.) Inflammation: Basic Principals and Clinical Correlates. New York, USA.
- Freifeld A, Proia L, Andes D, Baddour LM, Blair J, et al. (2009) Voriconazole use for endemic fungal infections. Antimicrob Agents Chemother 53: 1648-1651.
- Fortaleza SCB, Lopes SKDA, Bandeira TDJ, Neuma T, et al. (2004) Acute disseminated histoplasmosis in an immunocompetent patient. J bras pneumol 30.
- Wheat J, Sarosi G, McKinsey D, Hamill R, Bradsher R, et al. (2000) Guidelines for Management of Patients with Histoplasmosis. Clinical Infectious Diseases 30: 688-695.
- Kabangila R, Semvua K, Rambau P, Jackson K, Mshana SE, et al. (2011) Pulmonaryhistoplasmosis presenting as chronic productive cough, fever, and massive unilateral consolidation in a 15-year-old immune-competent boy: a case report. J Med Case Rep 5: 374.
- Brickner JP, Muenster JE, Pancoast TH, Tosh AK (2014) An adolescent with asthma presenting with worsening cough. Int J Adolesc Med Health.
- Disalvo AF, Bigler WJ, Ajello L, Johnson JE, Palmer J (1970) Bat and soil studies for sources of histoplasmosis in Florida. Public Health Rep 85: 1063-1069.
- Bahr NC, Antinori S, Wheat LJ, Sarosi GA (2015) Histoplasmosis Infections Worldwide: Thinking Outside of the Ohio River Valley. Current Tropical Medicine Reports 2: 70-80.
- Hage CA, Knox KS, Wheat LJ (2012) Endemic mycoses: overlooked causes of community acquired pneumonia. Respir Med 106: 769-776.
- Wheat LJ, Conces D, Allen SD, Blue-Hnidy D, Loyd J (2004) Pulmonary histoplasmosis syndromes: recognition, diagnosis, and management. SeminRespirCrit Care Med 25: 129-144.
- Gulati M, Saint S, Tierney LM Jr (2000) Clinical problem-solving. Impatient inpatient care. N Engl J Med 342: 37-40.
- Swartzentruber S, Rhodes L, Kurkjian K, Zahn M, Brandt ME, et al. (2009) Diagnosis of acute pulmonary histoplasmosis by antigen detection. Clin Infect Dis 49: 1878-1882.
- Hage CA, Azar MM, Bahr N, Loyd J, Wheat LJ (2015) Histoplasmosis: Up-to-Date Evidence-Based, Approach to Diagnosis and Management. SeminRespirCrit Care Med 36: 729–745.
- Babady NE, Buckwalter SP, Hall L, Febre KML, Binnicker MJ, et al. (2011) Detection of Blastomycesdermatitidis and Histoplasmacapsulatum from culture isolates and clinical specimens by use of real-time PCR. J ClinMicrobiol 49: 3204-3208.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences